
Diagnosis
I learned I had breast cancer on Feb. 13, 2023. I spent a good hour on the phone at midnight after work crying with one of my best friends trying to process it all and the uncertainty at that point. I didn’t know what stage, I didn’t know what kind, I didn’t know how bad it was, I didn’t know what I was going to tell my teenagers. (well, 18 and 20)
Having an education in mammography meant I was already one step ahead with understanding a lot of the technical stuff.
I got my official diagnosis via phone call by my radiologist on Valentines day. Definitely no longer a favorite holiday! He was at least reassuring that even though it was going to be a rough road I was “going to be just fine.”
That first 48 hours was one of the 2 hardest blocks of time to get through. Processing it all:
Why me?
How did this happen?
I’m a cancer patient now?!
What will I tell my kids?
What’s going to happen to me?
I’m really young to have breast cancer!
It took me 2 days to get tired of “processing” it. I knew I had to change my attitude because that was the one thing I could control!
“I can’t undo it, I can’t change it, it’s not going to go away! OK, fine! Lets do this! I can do this! <I think>”
Work
I was at least lucky enough that I didn’t have to work if I didn’t want to. And I didn’t want to. At that point I asked the scheduler to take me off the schedule until I figured all this out. When I learned how long my treatment plan was I told my boss I’d like to terminate my employment and I’ll revisit this after I get through everything. She was very understanding.
One Option
The first two weeks was a whirlwind of appointments, all moving so fast. My radiologist referred me to a breast surgeon who would be my team lead. I had my consultation within a week of my diagnosis. She explained my cancer and followed with my treatment plan saying, “this is what you’re going to do if you want to live and you’re going to start NOW!” It wasn’t open for discussion and I didn’t have time to think about it. There weren’t “options” there was just one! Of course, it’s my body I could have protested if I wanted to, but when you hear those words you tend to not argue after that.
Treatment
Chemo, double mastectomy (with or without reconstruction, my choice), lymph node removal (how many would be determined in my surgery), radiation therapy was on the table as a maybe at that point, and anti cancer injections for a year. In that order.
I was to get chemo first followed by my double mastectomy. This was so we could watch the tumors and see if they were going down and responding to the chemo and also check the pathology of the tissue to make sure it was really gone. If the surgery happened first we wouldn’t know if it responded to the chemo.
Getting Started
In the next 2 weeks I had 3 CT scans, 2 MRIs, a consultation with my oncologist, an echocardiogram, lab work, surgery for a chest port placement and I was sitting in my first chemo treatment by that second Friday. I have never seen the medical field move so fast before, even having worked in that field a bit. All my tests going forward were read and posted to my patient portal within 2 hours.
Except for my scans to see what stage I was.
I knew from a positive lymph node biopsy that I was advanced, at least stage 3, but I didn’t know if it spread further. I had a breast MRI on a Friday and appointments for a brain MRI, chest, abdomen and pelvic CT scans on Saturday morning. The radiology department is closed on Saturdays. I had the whole department to myself for 4 hours.
Because it was a weekend I didn’t get my tests read right away. I had 2 of the longest days of my life wondering how far it spread, what was going to happen and what I was going to tell my kids. A whole weekend imagining if this meant I would be leaving them without a mother for the rest of their lives. Even as “adults” I knew how hard that would be on them. I lost my mom to cancer when I was 15 and the thought was unbearable.
Stage 3
I was sitting in the waiting room at the surgery center Monday morning waiting to have a chest port put in when I got the phone call from my breast surgeons office. All my scans came back clean and it hadn’t spread further than the lymph nodes! I was so relieved I didn’t care what happened after that. I no longer felt like my time was limited. I really felt like I actually COULD do this! Surrender to my treatment plan and eventually get back to my life with my loved ones. It was going to be a long year, but I could do it!
People ask me what was the hardest part of it all. Those 2 blocks of 48 hours were the worst! Accepting the news and waiting to see how far it spread. For the most part I handled the whole thing pretty well. I had 2 occasions where I just finished grocery shopping, put everything in the car and as soon as I got into the driver’s seat I started crying. I didn’t even see it coming either time. I wasn’t actually thinking about it at the time but I guess I had some feelings that needed to come out. I’m not usually emotional in front of others so it makes sense that in a private space in my car when my errands were done was where it was all going to come out. Looking back, only twice for 10 minutes each (after my initial 48 hours of falling apart) for a cancer diagnosis- I’d say I handled things pretty well emotionally.
My Chest Port Surgery
This would be my first surgery, ever! I thought I would be more nervous as I have always been petrified of the thought of having surgery, but in the grand scheme of things going on at the time it actually seemed pretty small. I just got the only good news I had heard in the past couple weeks and was so relieved that I didn’t even care about my surgery.
After some time in the cardiology department prepping for my surgery I was taken back to the OR. I was informed that I would be awake for the whole thing, they were only going to give me enough general anesthesia to make me comfortable but not out. I didn’t like the sound of this but it wasn’t as bad as I thought.
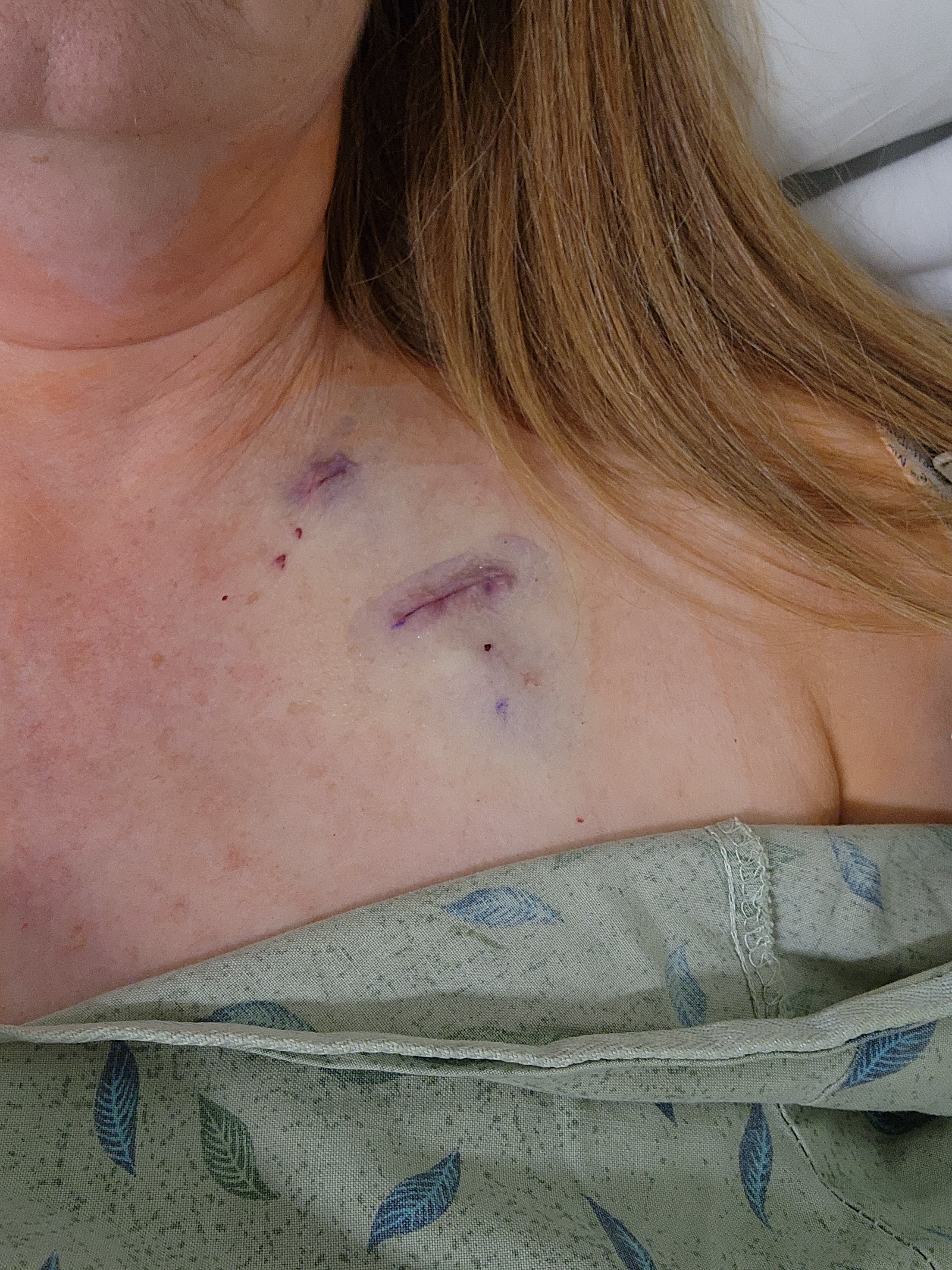
They draped me, cleaned me, prepped me and made a little tent over my head and face where I could only see the anesthesiologist. The anesthesia was just enough to make my vision blurry, but that was all. After some local anesthesia and 2 incisions, one above and one below the collarbone, the doctor created a little pocket under my skin for my port to sit and ran the catheter tube that was connected to it up over my collarbone and into my jugular vein. He then tunneled the tube through my jugular to the entrance of my heart. Because I wasn’t given much general anesthesia and he did local only on the left side, as soon as the tube crossed under my sternum to the right side I felt pain as he pushed the tube the rest of the way. Thankfully it was over quickly. The tube was cut to size so it ended just before the heart valve. They said usually they put the chest port on the right side because it’s closer to the heart entrance, but my cancer was on the right and they wanted to keep it out of the way so they put mine on the left.
The chest port is so the meds would be injected straight into the heart and distributed throughout my body instead of into one single vein all at once. I’m told chemo meds will destroy veins. My first infusion was in the vein on the back of my hand because my port didn’t work and that hurt for weeks and left a dark discoloration for a while. I can’t imagine doing all of them this way.
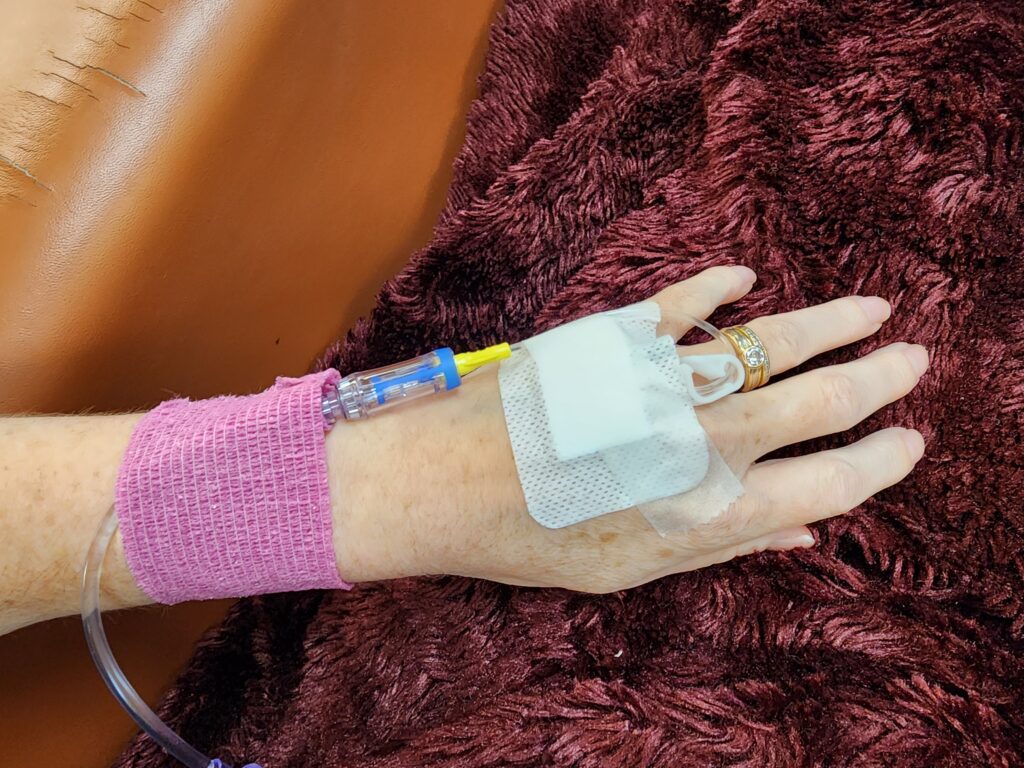
After gluing my incisions closed I spent an hour in recovery and was sent home that afternoon. It took 3-4 hours total to do 1 ten minute procedure. The port where they stick the needle is just below the lower incision. It took me a while before I was comfortable touching it. I could also feel the tube wrapping over my collarbone and that was definitely creepy!
My Team
My breast surgeon was in charge of creating a team of doctors that would see me through. I soon had an oncologist, plastic surgeon and radiation oncologist added to my team that would all work together doing their part when the time came.
Of course I couldn’t have gotten through it all without all the radiologists, mammography techs, x-ray techs, nurses, radiation therapists, medical assistants, surgical assistants and clinical staff that also played a huge part in my treatment!
First up, the oncologist and chemotherapy!
